How do MAO inhibitors work and why are they dangerous?
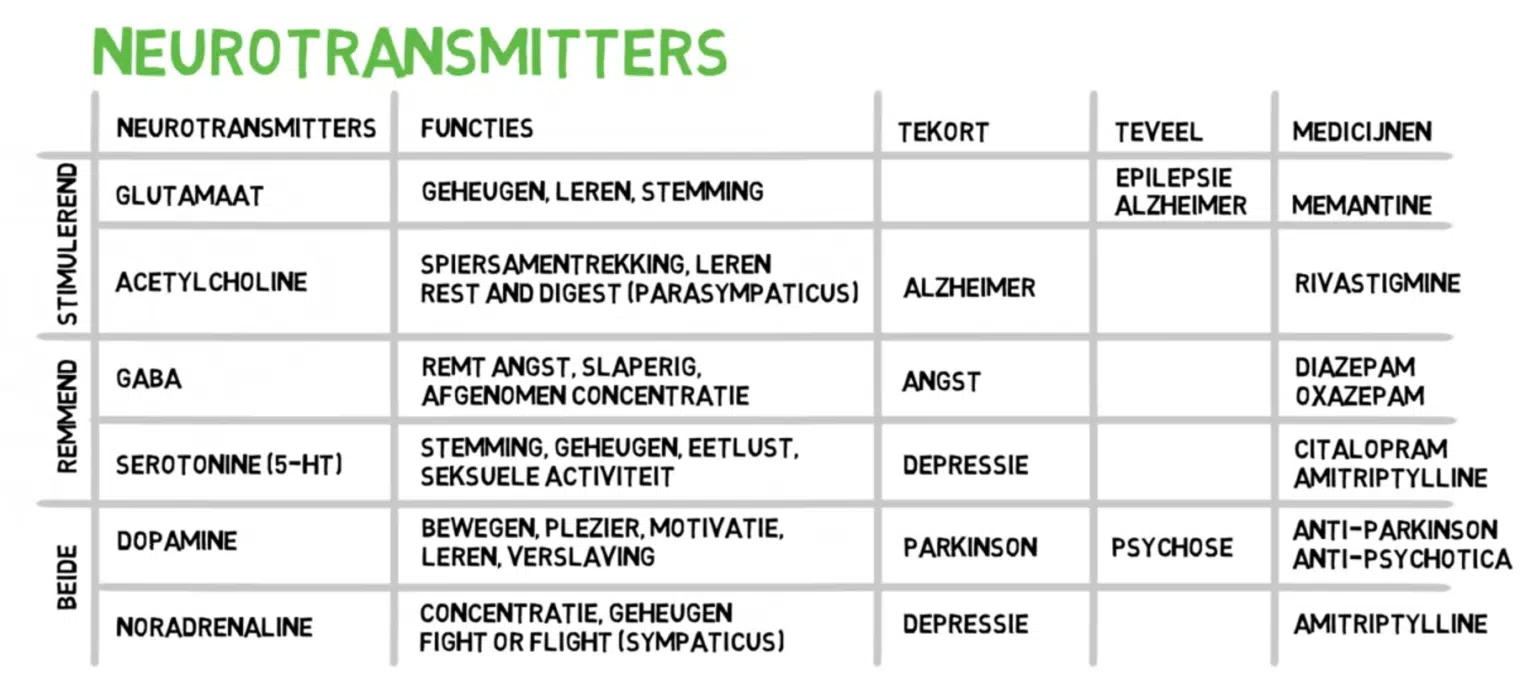
MAO inhibitors, or monoamine oxidase inhibitors, are substances that block the action of the enzyme monoamine oxidase (MAO). This enzyme is responsible for the breakdown of various neurotransmitters, such as serotonin, dopamine, and norepinephrine, as well as other monoamines such as tyramine. By inhibiting MAO, these substances can remain active in the body longer, which can lead to increased levels of these neurotransmitters. This mechanism is the basis for the use of MAO inhibitors in the treatment of depression and anxiety disorders, especially when other antidepressants are not effective.
- Non-selective MAO inhibitorsThese inhibitors block both MAO-A and MAO-B and are often prescribed for the treatment of depression. Examples include phenelzine and tranylcypromine.
- Selective MAO inhibitorsThese inhibitors specifically target one type of MAO enzyme. Examples include moclobemide, which primarily inhibits MAO-A.
- AyahuascaThis is a traditional South American drink that often DMT contains, a psychedelic substance that is rapidly broken down by MAO. In ayahuasca The plant Banisteriopsis caapi is often used, which is a strong MAO inhibitor, causing DMT to become orally active.
The cheese reaction:
- Serotonin syndromeCombining MAO inhibitors with serotonergic medications such as SSRIs (Selective serotonin reuptake inhibitors) and SNRIs (Selective serotonin and norepinephrine reuptake inhibitors) can lead to dangerously elevated serotonin levels, which the serotonin syndrome can cause.
- AntidepressantsThe use of TCAs (tricyclic antidepressants) in combination with MAO inhibitors is also risky.
- AntipsychoticsCombining MAO inhibitors with antipsychotics can also be dangerous.
- StimulantsThe use of amphetamines, cocaine, and other stimulants in combination with MAO inhibitors can lead to serious health risks.
- Alcohol: Alcohol use in combination with MAO inhibitors can also be dangerous.
- Medicines for high blood pressureCertain blood pressure medication can be problematic in combination with MAO inhibitors.
- OpioidsThe use of opiates such as tramadol, morphine, and codeine in combination with MAO inhibitors is very risky.
MAO inhibitors belong to the oldest classes of antidepressants, with a unique mechanism of action that offers both therapeutic potential and significant risks. By inhibiting monoamine oxidase (MAO)—a key enzyme in neurotransmitter breakdown—these agents modulate the availability of serotonin, norepinephrine, and dopamine. Nevertheless, their clinical use is limited by life-threatening interactions with tyramine-rich foods and serotonergic medications. This analysis highlights the pharmacodynamic principles and risk factors that make MAO inhibitors a "last-choice" agent for treatment-resistant depression.
Pharmacodynamic Basis of MAO Inhibition
Enzymatic Inhibition and Neurotransmitter Regulation
MAO inhibitors bind to the flavin adenosine dinucleotide (FAD) coenzyme of MAO, rendering the enzyme inactive.. This has two primary effects:
-
Increased synaptic neurotransmitter concentrationsSerotonin (5-HT), norepinephrine (NE), and dopamine (DA) accumulate in the synaptic cleft, which induces mood improvement in depressed patients..
-
Accumulation of peripheral monoaminesTyramine – a vasoactive substance in fermented foods – cannot be metabolized, leading to excessive (nor)adrenaline release.
The irreversible binding of classical MAO inhibitors (phenelzine, tranylcypromine) requires 2-3 weeks for enzyme regeneration, while reversible agents (moclobemide) have shorter washout periods..
Isozyme Specificity and Clinical Relevance
MAO consists of two subtypes:
-
MAO-A: Primarily responsible for 5-HT and NE degradation, related to mood regulation
-
MAO-B: Focuses on DA and phenylethylamine, relevant to Parkinson's
Non-selective inhibitors (e.g., phenelzine) block both isozymes, which explains their broad effects as well as the risk of side effects. Selective MAO-B inhibitors (selegiline) have fewer dietary restrictions but a more limited antidepressant effect..
Hazards and Side Effects Profile
Hypertensive Crisis: The "Cheese Effect""
Tyramine – present in fermented products (aged cheese, salami, soy sauce) – is normally broken down by MAO-A in the intestine and liver. With MAO inhibition:
-
Tyramine reaches systemic circulation
-
Induces massive NE release from presynaptic vesicles
-
Causes α1-adrenergic vasoconstriction and tachycardia
Clinically, this manifests as:
-
Throbbing occipital headache (97% of cases)
-
Systolic blood pressure >180 mmHg (86%)
-
Intracranial hemorrhages (4% mortality)
A case report describes a blood pressure increase to 240/130 mmHg after consumption of 50g cheddar cheese while using phenelzine..
Serotonin Syndrome: Deadly Synergy
Combination with serotonergic agents (SSRIs, MDMA, tramadol) leads to overstimulation of 5-HT1A/2A receptors. Diagnostic criteria include:
-
Triad: Mental status changes (agitation), neuromuscular hyperactivity (tremor, clonus), autonomic instability (hyperthermia >38.5°C)
Pathophysiological mechanism:
-
MAO inhibition → 5-HT accumulation
-
SSRIs block SERT transporters → further 5-HT increase
-
Overactivation of postsynaptic receptors → malignant hyperthermia
A study recorded mortality rates of 2-12% in untreated cases, with risks peaking within 6-8 hours after exposure.
Autonomic and Central Side Effects
Frequent side effects according to the Pharmacotherapeutic Compass:
-
Orthostatic hypotension (62% prevalence): Due to peripheral DA accumulation and vasodilation
-
Anticholinergic effects: Dry mouth (45%), constipation (33%)
-
Sleep-wake disorders: Paradoxical insomnia despite daytime sedation
Rarer complications:
-
Dopaminergic toxicity: Psychosis exacerbation in schizophrenia (RR 3.1)
-
GABAergic dysregulation: Myoclonus and hyperreflexia
Interaction issues and contraindications
Pharmacokinetic Interactions
MAO inhibitors interfere with CYP450 enzymes:
-
CYP2D6 inhibition: Increases concentrations of β-blockers (metoprolol) and antipsychotics (risperidone)
-
CYP3A4 induction: Reduces the effectiveness of oral contraceptives
An interaction study showed a fourfold increase in AUC of dextromethorphan when combined with tranylcypromine..
Absolute Contraindications
-
Serotonergic agents: SSRIs, SNRIs, triptans (at least 5 weeks washout)
-
Sympathomimetics: Amphetamines, cocaine (risk of hypertension)
-
Central analgesia: Meperidine, tramadol (serotonin syndrome)
Case reports describe fatal interactions between MAO inhibitors and:
-
Linezolid (antibiotic with MAO-inhibiting activity)
-
MDMA (recreational use, 87% mortality with concomitant intake)
Therapeutic Policy and Monitoring
Dietary restrictions
A low-tyramine diet (<10 mg/day) is essential, with avoidance of:
-
Aged cheeses (cheddar, brie: 150-500 mg tyramine/100g)
-
Fermented fish (surströmming: 350 mg/100g)
-
Certain alcoholic beverages (Chianti wine: 25 mg/L)
Patient education should focus on hidden sources such as overripe avocados (35 mg/100g) and soy sauce (120 mg/15ml).
Acute Complication Treatment
Hypertensive crisis:
-
First choice: Phentolamine (α-blocker) 5-10 mg IV
-
Alternative: Nitroprusside 0.5-10 μg/kg/min
Serotonin syndrome:
-
Cyproheptadine (5-HT2A antagonist): 12 mg orally, followed by 2 mg every hour until control
-
Cooling and benzodiazepines for agitation
Conclusion
MAO inhibitors represent a double-edged sword in psychopharmacology. Although effective in treatment-resistant depression, their use requires strict dietary control, interaction monitoring, and patient education. The risks of hypertensive crises and serotonin syndrome underscore the importance of reserving them for specialized settings. Future developments in pharmacogenetics (CYP2D6 genotyping) and more selective MAO-B inhibitors may potentially improve the safety profile.