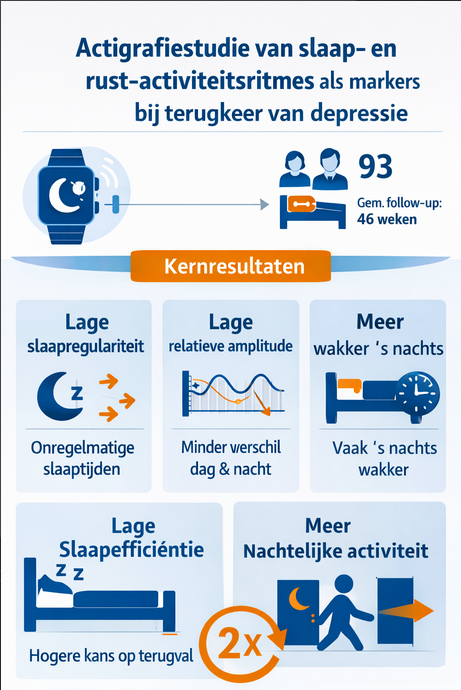
The study “One-Year Actigraphy Study of Sleep and Rest-Activity Rhythms as Markers of Relapse in Depression” investigated whether objective measurements of sleep and rest-activity rhythms via actigraphy can predict who will relapse into depression. It was an observational cohort study in Canada, with data collection from July 2016 to January 2019. The researchers followed 93 adults with a history of major depression who were relatively stable at baseline, with a MADRS score of 14 or lower. Together, they provided approximately 32,000 complete actigraphy days, with a median follow-up of 46 weeks.JAMA Network)
The primary outcome was relapse of depression. This was strictly defined as a MADRS score of 22 or higher for two consecutive weeks, or psychiatric admission, or suicidal intent or behavior, or escalation of antidepressant treatment. Actigraphic data were collected continuously and averaged over two-week periods.
The main finding was that a less stable sleep-activity rhythm was associated with a significantly higher risk of relapse. Lower sleep regularity, lower relative amplitude, lower sleep efficiency, and conversely more wake-after-sleep onset and more nocturnal activity were all associated with approximately a doubled risk of relapse. Of these variables, a lower relative amplitude remained particularly predictive, even after the researchers corrected for concomitant depressive symptoms.
The study therefore does not show that poor sleep is the cause of relapse, but rather that sleep and rhythm disorders can be clinically relevant biomarkers. The practical message is that depression is not just a matter of mood, but also of biological rhythm, sleep continuity, and day-night structure. According to the authors, these types of digital measurements could be deployed on a scalable basis for relapse monitoring.
Would psilocybin plus lifestyle coaching, with an emphasis on sleep, work better?
The strongest argument at this moment is not that this combination has already been definitively proven, but rather that various lines of research align. First, the JAMA study mentioned above demonstrates that sleep regularity, rhythm amplitude, and nocturnal restlessness are specifically associated with depression relapse. Second, meta-analyses show that improving sleep is indeed associated with better mental health and fewer depressive symptoms, and that treatment of insomnia in people with depression has, on average, a positive effect on mood. The recent European Insomnia Guideline therefore continues to recommend CBT-I as the first choice for chronic insomnia.
For psilocybin itself, the antidepressant signal is real, but not simple. In the 2023 JAMA study involving 104 adults with MDD, a single dose of 25 mg psilocybin with psychological support resulted in a rapid and sustained improvement in depression scores compared to active placebo. At the same time, the recent EPISODE trial in 144 adults with treatment-resistant depression was mixed: the primary endpoint was not significant, but the secondary outcomes did indicate clinically meaningful symptom reduction for 25 mg psilocybin. This means that psilocybin remains promising, but that optimization of context, preparation, and aftercare is likely important.JAMA Network)
That is precisely where sleep suddenly becomes interesting. A recent open-access analysis of 653 participants in guided psilocybin experiences showed that both depressive symptoms and sleep disturbances decreased after psilocybin, but that the improvement in sleep was smaller than the improvement in mood. More importantly, more severe sleep disturbances at baseline were associated with a lower likelihood of remission, and residual sleep complaints after the session predicted later depressive symptoms better than the reverse. The authors therefore explicitly conclude that addressing sleep disturbances may improve the therapeutic outcome of psilocybin.PMC)
This creates the most current and substantively strong argument for psilocybin plus lifestyle coaching. If sleep disturbance is associated with depression relapse, if improving sleep can improve mental health, and if sleep complaints are also associated with a lower chance of remission after psilocybin, then it is logical not to view psilocybin as a standalone intervention but as part of a broader recovery protocol. In such a protocol, lifestyle coaching should focus primarily on sleep regularity, sufficient daylight and morning activation, limiting alcohol and disruptive substances, stable eating and bedtimes, and, where necessary, CBT-I-like interventions. This is currently the best-substantiated reasoning, even though it is not yet a definitively proven treatment model.
No evidence
Based on current research, we cannot definitively prove anything. Specifically, there is no randomized study that directly compares psilocybin plus targeted lifestyle coaching for sleep with psilocybin without that coaching. The current substantiation is therefore primarily a synthesis of multiple studies, not a single conclusive trial. This makes the hypothesis strong and clinically logical, but not yet definitively proven. Specific research is therefore needed.
Conclusion
A current and well-defensible view is that psilocybin likely yields the greatest return when embedded in guidance that also strengthens the biological preconditions for recovery. Sleep appears to be one of the key targets in this regard, as disturbed sleep and disrupted circadian rhythms are associated with depression relapse, while sleep complaints also seem to predict a less favorable response to psilocybin. Based on this logic, psilocybin plus lifestyle coaching regarding sleep is not isolated speculation, but a plausible next step in the further development of effective treatment protocols.
See also: Natural remedies for better sleep around psilocybin sessions